
Adapt and Innovate
This article first appeared in the DukeMed Alumni News Fall 2020 issue.
Last spring, when Prince Boadi accepted an offer to attend Duke University School of Medicine starting in the fall of 2020, he knew the experience—leaving his family and friends in Chicago, learning his way around Durham, meeting new people, and taking on the rigors of medical school—would be different from anything else he’d ever done.
He just didn’t expect it to be quite this different.
“I’m pretty sure nobody has ever started medical school quite like this,” Boadi says of the first-year class. “Everybody is eager for things to get back to normal. But the faculty have been amazing, and we’re all learning to adapt. Even with all the challenges, I know there are a thousand people who would love to be in my position. I’m just glad to be here.”
Boadi and the other 600-plus new learners in the health professions and biomedical sciences have begun their education at Duke amid the worst global pandemic in a century. COVID-19 has affected almost every facet of life at the School of Medicine. The threat posed by the novel coronavirus has changed how students learn, how faculty teach, how scientists conduct research, and how clinicians care for patients.
The School of Medicine, along with the Duke University Health System and the university as a whole, has responded to the pandemic by rapidly reconfiguring a very large, complex institution to continue to carry out its core missions.
“Our faculty, staff, and students have responded superbly,” says School of Medicine Dean Mary E. Klotman, BS’76, MD’80, HS’80-’85. “We talk about innovation a lot. This challenge has required us to innovate on a massive scale, and our faculty have been remarkably creative and resilient in creating ways to carry on our work under extremely challenging conditions.”
Those changes range from new ways to deliver patient care to an expansive new multi-disciplinary course for students called “Responding to Pandemics: Past, Present, and Future,” which Alison Clay, MD, HS’02-’05, and Nancy Knudsen, MD, HS’92-’96, created with astonishing rapidity over the span of just a few weeks in early March.
A Proactive Plan
When the pandemic arrived in Durham in mid-semester last March, prompting the university to move all instruction online, close most research labs—except those focused on COVID-19—and restrict campus facilities, School of Medicine leadership scrambled to revamp the education and training programs. The summer break offered a bit of breathing room so that, in conjunction with Duke University and the Duke University Health System, they could assess, refine, and implement policies in preparation for the mass of students to return in August.
Medical school education leaders crafted a plan designed to allow students to gain the skills, knowledge, and experience required to advance toward their degrees on schedule while taking all practicable measures to prevent and minimize the potential spread of COVID-19 within the Duke and Durham communities.
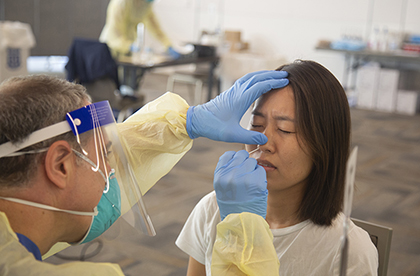
Mass COVID-19 testing of all incoming students, daily symptom monitoring for anyone going to campus, and widespread surveillance testing help quickly identify and isolate any cases of COVID-19 infection. Lectures, demonstrations, and projects are done via Zoom or other virtual platforms. Masks are required for in-person activities, and for close contact work, face shields offer additional protection. Student lounges and other common areas are off-limits; students go to campus or clinics only for required activities. Groups are subdivided and widely spaced and scheduled.
“Everything we can do remotely, we do remotely,” says Ed Buckley, BSE’72, MD’77, HS’77-’81, vice dean for education. “For the things we can’t do remotely, we implement all appropriate precautions: we wear PPE and meet in smaller groups in bigger rooms for shorter periods of time. We’re not crowding 15 people into a room on rounds; with technology like video iPads, not everybody has to be in the room at the same time to get the learning experience.”
Learning Despite Limitations
Thanks to these proactive measures, students are participating in most customary learning activities, albeit under obvious limitations. First-year students are watching lectures virtually, participating in team activities, and learning how to take medical histories and administer physical exams.
“At many medical schools, lectures are videotaped and posted online anyway,” says Maggie Min, a first-year medical student. “Even before COVID, a lot of medical students watched lectures online. The first-year curriculum is largely lecture-based, so if there’s ever a time to be stuck at home due to a pandemic, it’s this year.”

At the same time, COVID-19 has curtailed many of the usual activities—coffee shop meet-ups, football games, spontaneous conversations in the hall, and so on—that give students, especially new ones, the opportunity to get to know each other.
“That’s been the hardest part,” says Boadi. “Your first year is when you meet your classmates and really feel like you’re at Duke. We’re losing a lot of that. People are having Zoom get-togethers and small socially distant gatherings. It’s limited, but it helps.”
Clinical operations are back to near-normal volumes, and second-year students are rounding in smaller groups and gaining valuable experience participating in virtual “telehealth” visits with patients. Research labs are almost all open, and third-years are beginning their research projects with protective measures in place. Fourth-year students are doing their elective clinical rotations.

“A lot of medicine has moved to telehealth, but that can be difficult sometimes,” says Amy Petty, a fourth-year student in the Medical Scientist Training Program. “It’s hard to maintain six feet when you have to perform physical exams. We’re often examining people from a couple of inches away. The medical school provides us with masks and face shields, and they’re spreading us out among the clinics to keep providers, residents, and patients safe.”

A New Reality
The challenges and procedures vary by year and discipline. Ninety-four students are beginning their first year in the Doctor of Physical Therapy (DPT) program, the school’s second-largest student cohort, after the MD program.
“People who want to train as physical therapists are typically people who seek personal connections and caregiving,” says Tiffany Hilton, PT, PhD, assistant program director and director of curriculum for the DPT program. “The isolation and distancing have been difficult. Most of the first-years are in a new environment where they want to make connections, but that’s hard right now. But we’re doing everything we can to prioritize the student experience and give them the education they need to be excellent physical therapists.”
The constraints required by the pandemic can be cumbersome, says Glenda Holcomb, a second-year DPT student.

“When we practice physical therapy skills, some techniques require the subject to lie face down on the table, and that’s a bit awkward when you’re wearing a face shield,” Holcomb says. “But we’re all in the same boat, so that helps. I have my ‘village,’ my little group of friends, and we’re able to get together and study safely, practice skills, and so on. That’s important. It’s easy for your mental health to go haywire in these times, and you have to find ways to connect.”
The Duke Physician Assistant (PA) program, one of the largest in the country with a total of 180 students and nearly 40 faculty, had to rapidly revise its education and clinical rotation offerings last spring to meet the new reality.
“The wonderful curriculum that we had nicely prepared to deliver is not a remote, virtual curriculum,” says Program Director Jacqueline S. Barnett, DHSc, MHS, PA-C. “We did not want to try to force a square into a circle, but we had to take that square curriculum and chisel it into a circle to make it fit into this new virtual paradigm.”
The PA faculty has crafted a curriculum with virtual electives and scrambled to schedule rotations for clinical-year students. Some PA students chose a rotation working with the Durham County Department of Public Health to conduct COVID-19 contact tracing. Tara Blackley, MBA, MPH, deputy public health director of the Durham County Department of Public Health, called them “an incredible asset.” The incoming class of 92 PA students is doing mostly online instruction supplemented by small-group in-person activities. For in-person activities, students submit symptom monitoring and use appropriate PPE.
Hard-won Lessons
Exactly what the world will look like whenever the pandemic eases, nobody really knows. But across the School of Medicine, faculty are looking at this year as an opportunity to draw valuable lessons that will shape health care and medical education long after the 2020 pandemic has faded.
One obvious example is the explosion in the use of live streaming platforms like Zoom as a way to teach, meet, and provide health care remotely. COVID-19 accelerated the evolution of telehealth in a way that is probably here to stay; telemedicine patient visits have risen from a pre-pandemic level of about 100 per month to over 1,000 per day.
“Telemedicine was moving slowly because there was no driving force pushing it,” says Buckley. “The pandemic pushed it. It forced us to figure out the logistics and best practices. From here on out, I think you’re going to see a lot more telemedicine and remote learning, virtual meetings, academic events, grand rounds, and so on.”

COVID-19 has also—at a terrible cost—advanced the state of knowledge about infectious disease in ways that will resonate for years to come. Awful though it has been, this pandemic is helping prepare us for the next one.
“The next generation of physicians, having lived through this as students, will be better equipped for this kind of thing in the future,” says Buckley. “And we know this is not the last we’ll see of this kind of thing. We’re much better prepared now than we were a year ago, and in a year we’ll be better prepared than we are now.”
One other lesson the pandemic has taught: the importance of connection and communication, especially at times of stress.
“I think the students have helped keep us sane,” says the PA program's Barnett. “They have been so gracious and grateful for everything the program is doing to try to keep them on track. They have been just as worried about us as we have been about them.”

The concern goes both ways. The faculty know this is hard on students. Just saying that makes a difference.
“I really appreciate how much the School of Medicine acknowledges that this is a challenging time to be in medical school,” says Min. “They’ve told us repeatedly how much they appreciate that we decided to matriculate this year in spite of everything. Just having them say, ‘We know it’s difficult, but we’re very glad you’re here,’ means a lot.”
Top feature image: First-year Duke medical student Prince Boadi receives his white coat and stethoscope from Advisory Dean Leonor Corsino, MD, in the Trent Semans Center. Photo by Shawn Rocco.
Rhiannon Giles contributed to this story. All photos by Shawn Rocco, multimedia producer and senior media relations strategist for Duke Health. Story by Dave Hart, senior public relations specialist for Duke Health Development and Alumni Affairs and editor of DukeMed Alumni News.
