
For older adults who are homebound or those who have disabilities, it can be nearly impossible to make it to clinical and specialty appointments.
Patients may not have a ride. Or the ride they arranged doesn't show up. Other times, patients may not know they have an appointment. They don’t hear the phone ring or can’t retrieve voicemails.
When they do make the appointment, there is often not enough time. Sometimes the doctor is running behind, and the visit must be cut short because the patient’s ride has another obligation. Or the patient may be dropped off late or forgot to bring their medications. These disruptions in care make it harder for doctors to get to know their patients and allow them to be easily labeled as difficult and uninterested in their own care.
Duke University medical students launched a first-of-its-kind telehealth program that not only debunked that belief but also transformed the way primary care was delivered to low-income older, homebound adults, and those with disabilities in Durham.
“In home care is life-enhancing for homebound people and life-changing for those of us who do the work,” said Howard Eisenson, MD, former Medical Director of Lincoln Community Health Center and medical professor in Duke’s Department of Family Medicine and Community Health.

A study about the program, published this month in the Journal of General Internal Medicine, found that having students conduct in-person visits with these patients in their homes while a clinician supervised the visit virtually increased patient access to consistent, personalized care, and provided students with a uniquely fulfilling learning experience.
“How their homes were set up, how the kitchen and living rooms were positioned, the bright light bursting through some, and the darkness that filled others — that’s what sticks with me,” said Kelly Goo, MD, MPH, a graduate of Duke School of Medicine’s Primary Care Leadership Track.
Goo and Eisenson, the clinician who supervised student visits, led the program together. They enrolled eight patients with multiple chronic illnesses into the study, which ran from November 2022 to June 2023. All of them are participating in Lincoln Community Health Center’s Just for Us program, which provides medical care to homebound adults in Durham. A first year and third year student were paired with each patient.

Patients suffered from a various combination of chronic heart or lung disease, diabetes, pain, degenerative arthritis, neurological disorders like Parkinson’s or Multiple Sclerosis, and mood disorders.
During the first visit, Eisenson accompanied the students to the patients’ home. The following month students used a wireless hotspot to connect to Eisenson, who supervised the appointment virtually. He re-joined in-person the month after and continued this rotation for the rest of the program.
Student teams measured blood pressure and oxygen levels, checked blood sugar, collected medical histories, and reviewed medication regimens with patients and caregivers. “It exposed them to the specialness of in-home care, and gave students a bit of autonomy,” Eisenson said.
They found practical ways to make care more accessible. Goo once pulled up a ‘how-to’ video on her phone to show a patient how to use their inhaler, while Eisenson would set up medication trays for those with limited mobility.
The program revealed the true depth of the obstacles these patients face every day. “Having those snapshots into their lives solidified how much of health care we don't see in the interactions we have with patients in clinic, and how much people have to navigate on their own,” Goo said.
Every encounter further grounded the team in compassion. “You begin to appreciate not just their challenges, but also their resources, strengths, and resilience. You start to see them as real people and more than just another case. It's more satisfying and fulfilling to take care of people when you see them as people, and not as a particularly difficult case,” Eisenson said. “It builds trust, mutual regard and even affection.”
The teams didn’t just get to know the patients; they bonded with family members, neighbors, and pets. “When you see them in the home with a family member, you can recognize the importance of that family member, and you can congratulate them on the work they're doing, and you can reinforce what they're doing,” Eisenson said.
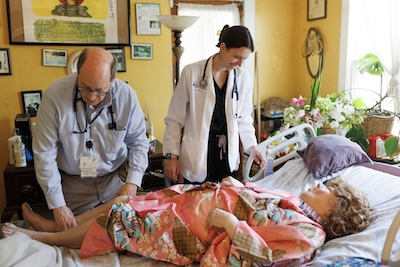
Visits lasted up to an hour, and that time was a luxury. “We’re not on the same production line as the one in the office, and we don’t spend the day apologizing for being behind,” Eisenson said.
This relaxed environment gave students the space to gain a better understanding of their patients and their past experiences, which helped them develop more informed and personalized treatment plans.
“We had to recognize the mental load the patients were carrying from the trauma of chronic illness, acknowledge how past traumas affected their ability to manage current health conditions, and cope with new diagnoses, to see how we could help and make things as straightforward and feasible for them as possible,” Goo said.