
Duke Researchers Pivot to Attack the New Coronavirus
In the race to understand the new coronavirus and generate solutions, Duke research teams are well underway.
In fact, you could say they’ve been working on it for decades. Everything Duke experts have learned over the years about the spread of new diseases, the biology of viruses, and the techniques of developing treatments and vaccines is now being applied to the new coronavirus, SARS-CoV-2, and the illness it causes, COVID-19.
These experts work across the medical school and campus as well as abroad. They work in the Duke Human Vaccine Institute (DHVI), the Duke Global Health Institute (DGHI), and the Duke-NUS Medical School in Singapore, among many other centers, institutes, and departments. And they are collaborating with other experts across the globe.
Duke also has state-of-the-art facilities—some of which are uncommon on university campuses—that are speeding up the development of new treatments and vaccines.
“We’ve got years of experience working with viruses and other pathogens,” says Colin Duckett, PhD, vice dean for basic science in the School of Medicine. “Because we have the infrastructure and highly trained experts, we’ve been able to pivot rapidly to confront this new challenge.”
Slowing the Spread
Epidemiologists and those who work in global health are hard at work learning more about how the virus spreads, with the immediate goal of slowing the spread.
“If we string out cases over time, especially for those likely to have severe disease, our intensive care units won’t be overrun and we can help them survive,” says Gregory Gray, MD, MPH, FIDSA, professor of medicine in the Division of Infectious Diseases and member of the Duke Global Health Institute. He also has appointments at Duke-NUS Medical School in Singapore, Duke Kunshan University in China, and the Duke Nicholas School for the Environment.
Gray’s lab members are conducting investigations both in Durham and Singapore to discover how far the virus can travel in the air. The investigators are setting up bio-aerosol samplers at various distances from patient beds to collect and identify virus and virus particles. Current thinking suggests the virus doesn’t typically travel beyond 2 meters (6 feet) from an infected person; Gray’s studies will help confirm or revise this.
Gray, an epidemiologist, is also working to collect and analyze data related to close contacts of infected people to learn more about the incubation period and what sorts of interactions are likely to result in transmission. Refining those two pieces of information will improve mathematical models of the spread.
In the lab, Gray’s team is starting work to identify animal reservoirs, which are animals in which a virus multiplies prolifically, often without causing symptoms. The etiology of SARS-CoV-2 hasn’t been nailed down, but it may have started in bats as some other coronaviruses have, and then become amplified in animals that have more contact with humans, perhaps wild animals in markets or domesticated livestock. In any case, if animal reservoirs can be identified, limiting or modifying contact with those animals can slow the spread.
Diagnosis
Faced with rapid spread of disease and a limited supply of test kits available to the state, a variety of private labs and universities, including Duke and UNC Chapel Hill, quickly developed their own tests for SARS-CoV-2. These tests provide a yes-or-no response to quickly identify patients who have been infected.
Other types of tests will be needed to facilitate treatment and research. For example, knowing how much virus is present could be useful. These kinds of assays are often used for HIV, where “viral load” guides treatment decisions.
The lab of Thomas Denny, chief operating officer of DHVI, develops these kinds of assays and assay validations in support of HIV clinical trials. Denny says the National Institute of Allergy and Infectious Diseases (NIAID) asked his lab and other labs it funds focusing on HIV assays to shift to the new coronavirus.
“We have expertise that can flip over and develop assays for other viruses,” he says. “It’s a frame shift. We’ve been doing things similar to this for HIV, for H1N1 and other flu viruses, and now we’re working to do that for this virus.”

Denny Lab, harvests lymphocytes under
BSL-3 conditions in the Duke Regional
Biocontainment Laboratory. These cells are
from someone who has COVID-19 and will
be used to study how the virus interacts with
the immune system of the individual who is
infected.
Denny and others in DHVI work with partners in African countries, which have the potential to be hit hard by the combination of SARS-CoV-2 and high rates of HIV. Denny and others are anxious to share assays with those labs to help them respond to the new disease.
Denny’s lab is also helping to validate assays created by others, including the University of Texas Medical Branch in Galveston. Speed was of the essence to help respond to the shortage of tests kits from the CDC. “Our work with the UT team was to get that done quickly so there would be an approved test kit that other institutions or labs could [use],” he says.
Treatments and Countermeasures
Duke has been approved to participate in a nationwide clinical trial sponsored by NIAID evaluating remdesivir in patients hospitalized at Duke University Hospital with COVID-19.
Remdesivir is a broad-spectrum antiviral drug that was developed for use with Ebola and has since shown some effectiveness against severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS), which are both coronaviruses.
Cameron Wolfe, MD, associate professor of Medicine, is the Duke lead on the trial. “The fact that our teams operationalized this substantive study in the space of a week or a week and a half is astonishingly fast-paced,” Wolfe says. “It is a credit to folks in multiple departments. There hasn’t been a single person who hasn’t rolled up their sleeves and said, ‘Let’s make this happen.’”
In addition to getting the studies off the ground quickly, Wolfe expects data will also be available quicker than usual. “Because of the incredible efforts of individual people trying to make it happen, and the adaptive nature of the trial, we would anticipate getting nationwide, actionable data in a matter of months, not the usual extended length of time,” he says.
Remdesivir is a so-called small molecule drug, as are most pharmaceuticals. A newer class of therapies are monoclonal antibodies, also called large-molecule drugs or biologics. These typically have the suffix “mab,” such as denosumab (Prolia) and pembrolizumab (Keytruda), and are given as injections or infusions rather than pills. Monoclonal antibodies may also prove to be a powerful tool in the fight against SARS-CoV-2.
Developing such a treatment is underway in the Duke Human Vaccine Institute (DHVI) in the lab of Greg Sempowski, PhD, professor of Medicine and Pathology. “My research program focuses on developing antibody treatments for viral pandemic pathogens,” he says. “This is a temporary treatment, or medical countermeasure, to help blunt or stop a pandemic in its tracks.”
An antibody treatment doesn’t confer lasting immunity as a vaccine does, but would help infected patients beat the disease. It also could be used as a temporary preventative for groups being exposed to the disease, such as healthcare providers or people in the military. “It’s something that would be a short-term measure while the vaccines are being developed, optimized and tested,” Sempowski says.
Sempowski’s lab is one of four nationwide that’s been funded for several years by the Defense Advanced Research Projects Agency (DARPA) to develop rapid responses to pandemics. That means, for any unknown virus, being able to isolate the virus and antibodies from humans that are infected, select the antibodies that can neutralize the virus, and engineer delivery methods for these antibodies.
DHVI has a state-of-the-art laboratory where highly trained specialized personnel work with potentially dangerous pathogens. The National Institutes of Health (NIH) funded the construction of 14 of these facilities about 15 years ago, including the one at Duke. “It’s a highly secure facility with redundant safety mechanisms so we can safely work with these materials to develop drugs, diagnostics, and therapeutics,” Sempowski says. “It’s an amazing resource for our region.”
The DHVI also has its own in-house Good Manufacturing Practices (GMP) facility, which makes small batches of vaccines and medical countermeasures for initial phase 1 clinical testing. This rapid and cost-effective in-house manufacturing saves precious time. The Duke University School of Medicine and DHVI also have robust clinical trials units, including the Duke Vaccine Trial Unit (DVTU), led by Emmanuel (Chip) Walter, MD.
“At DHVI, we’re able to use in-house resources to rapidly go from bench to bedside,” Sempowski says.
Sempowski is pursuing a new technique that’s faster than engineering the antibodies themselves: creating genetic blueprints for the antibodies, in the form of messenger RNA (mRNA). When the mRNA is injected, the body follows the encoded instructions to make the antibodies itself.
“Switching to RNA-based manufacturing and delivery could help accelerate manufacturing and delivery of both vaccines and countermeasures,” Sempowski says.
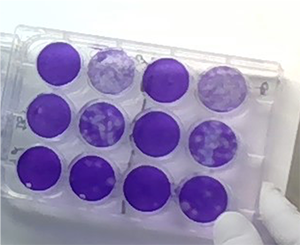
the cells (blue area) and also where the virus
has killed the cells (clear area). Courtesy of
Dr. Trey Oguin, Duke RBL Virology.
Vaccines
Vaccines are designed to prevent rather than treat an infection or disease. Used in a vaccine, mRNA would tell the body how to make fragments of the SARS-CoV-2 virus called spike proteins. These would spur the body to produce antibodies and “memory cells” that could respond if confronted with the actual virus later.
The vaccine effort at Duke is led by the director of DHVI, Barton Haynes, MD, the Frederic M. Hanes Professor of Medicine. Haynes has long worked to develop a vaccine for HIV, a notoriously sneaky and frequently mutating virus. He leads a multi-institution consortia that has received hundreds of millions of dollars in funding from NIAID and the Bill and Melinda Gates Foundation since 2005.
NIAID Director Anthony Fauci, who was an early mentor of Haynes, recently told Duke Magazine, “You’re dealing with a superstar who is leading a very impressive group of people. If we’re going to get a vaccine for HIV, it almost certainly is going to be all or in part by this group.”
Haynes is now turning his focus to SARS-CoV-2 in an attempt to develop a mRNA-based vaccine, using all the combined expertise of his team and the DHVI in-house production facility and clinical trials unit. In this effort, Haynes is collaborating closely with Drew Weissman, MD, PhD, professor of Medicine at the University of Pennsylvania.
“All of the past 15 years’ worth of work on the HIV vaccine has led to the development of the technologies that are now being used to rapidly respond to the COVID-19 pandemic,” Haynes said. “This includes the antibody-isolation technology we are using to isolate neutralizing antibodies and the rapid movement to vaccine and antibody production for clinical trials in our own vaccine production facility. Coupling these technologies with the state-of-the-art Regional Biocontainment Facility provides a powerful approach for rapid development of solutions to pandemics.”
Vice Dean Duckett says, “Bart Haynes is truly a pioneer in vaccine development, especially with his experience in HIV. His group is poised to make seminal contributions to the development of a vaccine for SARS-CoV-2.”
Preventing Future Pandemics
As an epidemiologist, Gray wants to be able to identify the next pandemic-causing virus before it causes a pandemic.
He is leading an effort to conduct a study at eight sites in six Asian countries to identify and keep tabs on zoonotic pathogens present in people who work in animal markets or who process meats. Benjamin Anderson, PhD, assistant professor of Global Health at Duke Kunshan University, will be leading the effort for three sites in China.
The immune systems of people who work closely with animals are repeatedly attacked or “insulted” by animal pathogens, but they usually are able to shrug it off. Sometimes, however, an animal pathogen adapts to life in a human host and gets better at multiplying in its new home. The real problem occurs when the pathogen begins moving from one human to another. “It’s a progression,” Gray says: “Insult, adaptation, effective replication, and then human-to-human transmission.”
The new project will harness genomic sequencing and big data tools to identify new pathogens that have adapted to the human respiratory tract and show transmission potential.
“That puts us ahead of the curve before the virus becomes highly effective at causing disease and human to human transmission,” Gray says. “If we can show that this works, it will be a novel tool that would help us get ahead of these outbreaks.”
Developing an Antibody Test
On the other side of the world, in Singapore, researchers at the Duke-NUS Medical School were among the first in the world to isolate the new virus, after China and Australia. They were also among the first, if not the first, to develop a blood test for antibodies to the virus, which makes it possible to identify people who have had COVID-19 even after they have recovered and cleared the virus.
The Duke-NUS Medical School was established in 2005 to provide graduate-level medical education in Singapore, which at the time had only medical schools that were designed for undergraduate-entry.
“We were brought by explicit invitation of the Singapore government to establish a research-intensive school that would train students to become clinician-scientists,” says Thomas Coffman, dean of the school. The school is organized around interdisciplinary public health issues, one of which is emerging infectious diseases, which are a particular concern for Singapore. “This region has been a fountain of new viruses,” Coffman says.
The school’s Programme in Emerging Infectious Diseases is directed by Linfa Wang, PhD. Wang is an expert in zoonotic viruses—those that jump from animals to humans, as SARS-CoV-2 did.
“I have been in this business for last 25 years,” Wang says. “This is my fifth emerging zoonotic disease outbreak and they all look like bat-borne viruses. We were ready [for the current outbreak] in many ways.”
Several years ago, Duke-NUS established a biocontainment facility (an animal biosafety level 3 laboratory) in Singapore, which has been a critical resource for work during the current outbreak. And Wang explicitly trains his lab members, doctoral students, postdocs, and junior faculty to be prepared for outbreaks.
“As a basic scientist, I think this concept of peace time and war time is so important,” he says. “I always tell my junior scientists: during peace time, publishing and working on your CV and grants are important, but during an outbreak, it’s about having an impact on the ground.”
Researchers at Duke-NUS, including Danielle Anderson, PhD, scientific director of the Duke-NUS biocontainment lab, isolated the live virus just days after receiving a sample from an infected patient at the end of January. Once the researchers had the virus and could grow it in the lab, they could begin developing a blood-based test to detect antibodies, called a serological test.
With that test in hand, the research team was able to use it to describe how a coronavirus outbreak in one church in Singapore led to an outbreak in another. A couple from one church, unknowingly infected, spent time with a man from the other church. Using the antibody test, researchers could determine that both members of the couple had indeed been infected with COVID-19 even though they were no longer symptomatic. One of them no longer had any virus in the bloodstream, so a standard SARS-CoV-2 test would have been negative.
Wang is setting up collaborations with research teams around the world on studies using the antibody test. In particular, it could be used to understand whether children are less likely to acquire COVID-19, or whether they simply don’t show symptoms. “If it’s the latter,” Wang says, “you can prove that by serology because even if the infection is mild, it still produces antibodies.”
Researchers at Duke-NUS will also be collaborating with others to test vaccines in clinical trials. Duke-NUS, in collaboration with the SingHealth team, has extensive clinical trials capacity, and Singapore, with its multi-ethnic population, is an ideal site. Wang is in conversations with the World Health Organization (WHO) and the Coalition for Epidemic Preparedness Innovations (CEPI) about potential vaccine trials.
Mary-Russell Roberson is a freelance writer in Durham. She covers the geriatrics and aging beat for the Department of Medicine in the Duke University School of Medicine.
