Is it possible for an adult brain to make new nerve cells? Scientists have debated this question for decades, with many concluding that neuron-making stops after childhood, or around the age of 13.
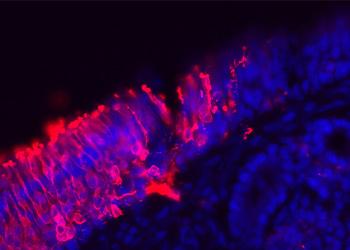
However, a research team recently rocked the debate again after finding a thriving neuron ‘nursery’ in a section of adult human nose tissue, the olfactory neuroepithelium. Neurons are the specialized cells in the brain designed to transmit information to other nerve cells and muscles. The olfactory area of the nose houses the neural receptors that give us the ability to smell.
Previously, studies had been limited to nasal tissue samples from mice. In the human samples used in the current study, the researchers found that immature neurons or “baby” neurons produced by stem cells represented more than half of the neurons in the tissue samples, suggesting that new neurons were produced in the tissue. The findings were published in the journal Nature Neuroscience. The finding has implications for correcting conditions that cause smell damage or loss, and add insights for treating the nervous system as a whole.
 Brad Goldstein
Brad Goldstein“We do not fully understand why people lose their sense of smell, which can occur for many reasons, and our data sets provide a wealth of information about the cell populations present in adult olfactory tissue,” said Brad Goldstein, MD, PhD, an associate professor and vice chair for research in the Department of Head and Neck Surgery and Communication Sciences, senior author of the study. “This is an important step in developing treatment strategies for conditions when this tissue may be damaged.”
Approximately one in eight Americans over age 40—up to 13.3 million people—have measurable smell dysfunction, according to the National Institute on Deafness and Other Communication Disorders.
“It will be very useful to use this window to analyze samples from people with conditions in which the nervous system has degeneration, such as Alzheimer’s disease,” said Goldstein. “Alzheimer’s is of particular interest, since these patients lose their sense of smell quite early in the disease process, and we have few treatments for Alzheimer’s disease. So, it may make sense to look carefully at regions of the olfactory system in these patients.”
Hiroaki Matsunami, Ph.D., a professor in the Department of Molecular Genetics and Microbiology and co-author on the paper, noted that while the researchers weren’t able to observe the neurons being made because of the nature of human samples, the molecular makeup of the immature neurons in the sample provide strong evidence that they were made in the nose during adulthood.
“Because the nose is exposed to the external environment, it might be possible we could one day collect these neuronal stem cells from patients and use them to treat their own brain disorders,” said Matsunami. “It is not outside of the realm of possibility.”
Other co-authors on the paper include Michael A. Durante, Stefan Kurtenbach, Zoukaa B. Sargi, J. William Harbour, Rhea Choi, Sarah Kurtenbach, and Garrett M. Goss.